More than 46,000 people are diagnosed with lung cancer in the UK every year, making it the third most common type of cancer. Our experts continue to push the boundaries, developing less invasive treatments to successfully treat complex lung cancers.
At Guy’s and St Thomas’ Specialist Care, patients with tumours in the lung can be treated using less invasive surgical approaches. In recent years, there has been a shift towards offering patients keyhole surgery and smaller incisions with no rib spreading.
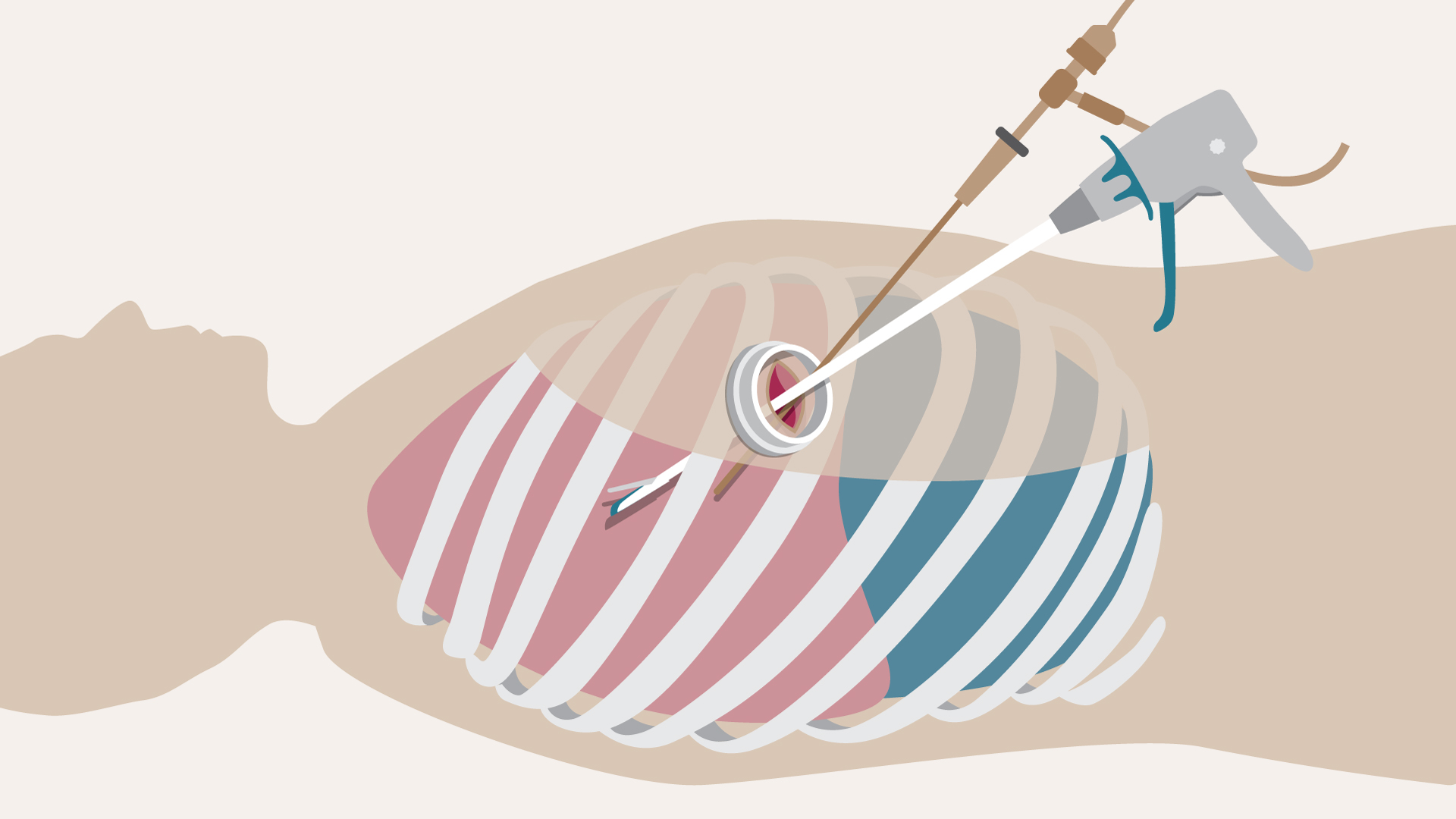
This approach is known as video-assisted thoracoscopic surgery (VATS) lobectomy. The experts at Royal Brompton Hospital believe the single port VATS lung resection technique allows for an even faster recovery and minimises complications, compared to conventional surgical approaches.
Because of the innovative treatment options offered at Royal Brompton and Harefield hospitals, patients who have been offered palliative treatments at their local hospital have sought a second opinion with us. Or, those patients who have been turned down for surgery elsewhere have had successful surgery at our hospitals.
World-class expertise
The lung cancer team at Royal Brompton Hospital work collaboratively with specialist oncology colleagues based at The Royal Marsden Hospital, ensuring every option is explored when planning treatment. This multidisciplinary approach is a team effort combining the expertise of world-leading specialists in their field.
Together the team provide their specialist knowledge in chemotherapy, radiotherapy and immunotherapy drugs and other treatment options. This allows for the best outcome for all patients.
If a patient requires surgery, the surgical team proceed without delay, backed up by the hospital’s world-class histopathology department. The expert team at Royal Brompton Hospital provide a world-class service and techniques that other centres in the UK do not practice.
Single port approach versus a traditional thoractomy
Benefits to the patient
- smaller incision and no rib spreading resulting in smaller, neat scars
- minimally invasive single port and multiport approaches heal very well
- post-operative pain is reduced and the recovery process is quicker
- most patients can return home after 5 to 7 days
Compared to 10 years ago, the conventional posterolateral thoracotomy has been significantly modified. With the minimally invasive single port approach, the length of the incision is much smaller and rib spreading is completely avoided. Both single port and multiport approaches generally heal very well with smaller, neat scars.
Mr Simon Jordan, consultant thoracic surgeon, explains: “We have found the use of single port minimally invasive surgery reduces the amount of post operative pain and speeds up the recovery process. It also allows the patient to have a more rapid return home.”
He continues, “Since this is a relatively new technique, the long-term benefits are still being investigated. However, this surgical approach is just as good as the conventional open chest surgery and probably confers benefit and allows more rapid recovery.”
“If the tumour is very big, then a thoracotomy would be the best approach, but most tumours are amenable to the minimally invasive single port technique.”
The risk of having a major complication is typically less than one per cent. Although this is major surgery, most patients are up and about the next day.
Successful outcomes
A recent review by an independent body examined all UK centres performing lung cancer surgery. The results concluded that Royal Brompton and Harefield hospitals have the highest lung cancer resection rates, treating the highest risk cases. The results included the single port VATS lobectomy approach, as well as multiple VATS and thoracotomy surgery.
Despite treating such high-risk cases, the two hospitals have achieved the best outcomes post-operatively and one year later. And when other patient risk factors and co-morbidities were taken into consideration, such as heart disease and heavy smoking history, the Royal Brompton and Harefield hospitals achieved the best one-year patient survival rates by far in the UK.
Lung cancer screenings
Increasingly, organised screening programmes or scans are picking up cancers, often at an earlier stage. Nationally and internationally, lung cancer screening is now widely available and can allow for diagnosis of cancers when they are most treatable, and surgery has a chance to be more curative.
Currently, more than two-thirds of lung cancers are diagnosed at a late stage, so survival rates for these patients are low.
Mr Jordan explains, “Historically we have recognised that only 10 to 20 per cent of lung cancers are surgically treatable or curable at diagnosis; this is typically following the development of symptoms.”
“But we hope with screening and lower dose CT scans that early stage lung cancers will be identified – even before symptoms develop.”
Our specialists run lung cancer screening clinics at both hospitals. The service is led by some of the UK’s leading specialists in respiratory medicine. The knowledge and expertise of our specialists and their teams are available to anyone with concerns about the risk of lung cancer.
Related content
-
Diagnostic tests for lung conditions
Our advanced, high-quality diagnostic facilities can help rapidly diagnose lung conditions.
-
Lung cancer
Lung cancer is a condition caused when the cells that make up the tissue of the lungs become abnormal and grow into a tumour.
-
Lung cancer risk assessment
Our world-leading specialists can assess your risk of developing lung cancer during a consultation.





