Children and teenagers usually experience mild or no symptoms with COVID-19 infection, but rarely it can trigger ‘PIMS-TS’ – a severe and potentially fatal inflammatory condition that requires urgent care. One of our world-leading paediatric cardiologists provides all the information parents need to know about this condition.
A rare condition requiring urgent care
During the UK’s first lockdown in 2020, a number of teenagers were admitted to the paediatric intensive care unit at Evelina London Children’s Hospital that were extremely unwell with no signs of an infection.
It would later emerge that, like other children and teenagers across the world, they were affected by a rare complication of COVID-19 infection. Their immune systems were overreacting to the virus leading to severe inflammation that affected multiple organs of their bodies, including their hearts.
This condition was later termed ‘paediatric inflammatory multi-system syndrome’ – or ‘PIMS-TS’ for short, a potentially fatal outcome of COVID-19 infection in children and teenagers.
What are the symptoms of PIMS-TS?
“We most often see PIMS-TS in those aged 8 to 15 and unfortunately its symptoms can be confused with other conditions such as appendicitis, which is also common in this age group,” explains Dr Carles Bautista, consultant paediatric and interventional cardiologist at Royal Brompton Hospital.
- aged 18 or under
- abnormally fast heart rate
- cracked lips and/or strawberry red tongue
- dizziness and low blood pressure
- headache
- tiredness and muscle pain
- infected with COVID-19 in the previous 4-6 weeks or contact with an infected person
- conjunctivitis (‘pink eye’) and/or widespread rash
- diarrhoea, tummy pain and vomiting
- prolonged high fever
- peeling of skin on hands and feet
“It is important that parents take their children to A&E as soon as possible if they suspect PIMS-TS. We are still learning about this condition, but what we do know is that the earlier a patient is admitted to hospital the better their outcomes are likely to be,” says Dr Bautista.
What increases the risk of PIMS-TS?
Our consultants from Evelina London Children’s Hospital (including our consultant in paediatric and fetal cardiology, Dr Owen Miller), led the world’s largest study on PIMS-TS across 55 centres in 17 European countries to better understand the condition and why it is caused.
Among other findings, the study demonstrated that patients from a BAME background were disproportionally affected, with almost a third of patients being from a black background.
Obesity was also another common factor for the development of PIMS-TS with 1 in 4 patients studied being obese. However, no other risk factor (including diabetes) was found to be associated.
Further studies have also shown that the variant of COVID-19 (strain of the virus) doesn’t influence whether someone develops PIMS-TS or not. It is therefore likely that a patient’s genetics can also play a part in developing the condition.
Dr Bautista, along with our consultant paediatric cardiologist Professor Alain Fraisse, have also published multiple articles on PIMS-TS.
Protecting Joseph’s heart
Joseph, aged 10, was experiencing bad tummy and back pain in April 2020. “He was a very healthy and sporty boy, playing football regularly and was rarely unwell, so I just immediately thought I needed to take him to A&E as this was really unusual for him,” explains Joseph’s mum, Elle.
“He couldn’t walk at all from the pain, so the doctors conducted some scans to see if it might be his appendix. He was also really sensitive to the hospital light and started developing a high fever which paracetamol wasn’t managing to bring down.”
The team at Princess Alexandra Hospital decided to keep Joseph in for further investigation, but his condition deteriorated rapidly. He received a positive test for COVID-19 infection and started showing signs of PIMS-TS, including a swollen strawberry red tongue and inflammation in his heart, prompting his transfer to St Mary’s Hospital’s intensive care unit for treatment.
“He was incredibly poorly and I just didn’t think COVID would affect his heart this way. But Dr Bautista was brilliant. He came to visit Joseph twice a day to check on and treat his heart. There are no words to describe how grateful I am to him and all the doctors and nurses at St.Mary’s and Royal Brompton Hospital in helping with Joseph’s recovery,” says Elle.
“It took Joseph a year to recover from his experiences in intensive care but he is now back to playing football again. He even raised over £1,000 for the NHS in a charity bike ride as a thank you for his treatment. We are incredibly proud of him.”
As PIMS-TS can affect multiple organs, a multi-disciplinary approach is needed for its successful treatment. Our paediatric cardiologists at Royal Brompton and Evelina London Children’s hospitals work in close partnership to provide the best care for patients. Together, they can provide a comprehensive service to quickly stabilise these very ill paediatric patients and utilise diverse specialist expertise for a total body approach to care.
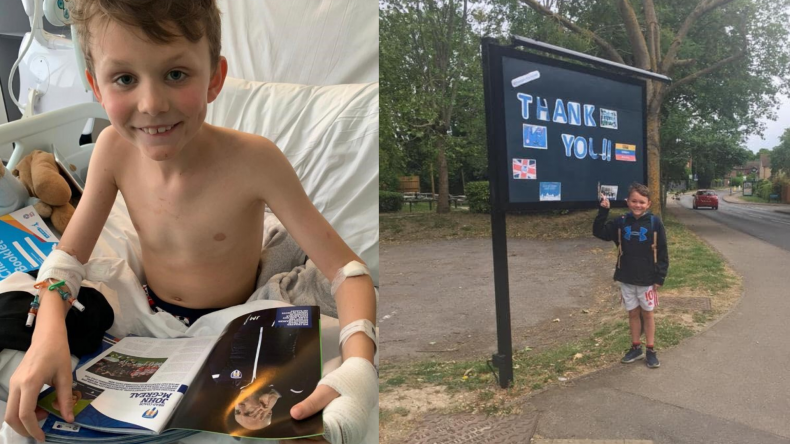
(L) Joseph recovering from PIMS-TS at St Mary's Hospital. (R) Joseph fully recovered and raising money for the NHS.


