COVID-19 infection in children and adolescents is often mild or asymptomatic, but rarely can trigger a multi-system inflammation disorder that requires urgent care. We provide the latest findings on the aetiology of PIMS-TS from the world’s largest study on the condition led by our consultants.
A rare syndrome requiring urgent care
In the middle of the UK’s first lockdown in 2020, a number of teenagers were admitted to the paediatric intensive care unit at Evelina London Children’s Hospital requiring inotropic support in the absence of infection.
It would later emerge that these teenagers, like others across the world, were affected by a complication of COVID-19 resulting in multi-system inflammatory disease, often leading to multiorgan failure and shock that required urgent intensive care.
This condition was defined and named ‘paediatric inflammatory multi-system syndrome temporally associated with SARS-CoV-2’ (PIMS-TS) by the Royal College of Paediatrics and Child Health in the UK, and MIS-C (multisystem inflammatory syndrome in children) by the WHO and CDC in the US.
What increases the risk of developing PIMS-TS?
Although it was originally described as a Kawasaki-like syndrome, the age of presentation for PIMS-TS is generally older. Where Kawasaki syndrome mostly affects children under 5, PIMS-TS presents with greater frequency in those aged 8-15. However, exactly how the infection trigger this syndrome is still unknown and it remains a rare outcome of COVID-19 infection in children and adolescents.
What is known is that the syndrome tends to appear 4-6 weeks after COVID-19 infection. Also, the COVID-19 infection is usually mild or asymptomatic, in-line with what is normally expected for these age groups (patients do not experience a more severe form of the infection before presenting with PIMS).
In terms of a mechanism of disease, it is thought that the viral spike protein may resemble a superantigen that can drive the development of a cytokine storm, triggering the multi-system inflammation observed with PIMS. Viral sequencing studies have also revealed that different strains of the virus do not influence the likelihood of the syndrome developing. It is therefore more likely that factors such as host genetics that trigger it.
To further understand the syndrome and its aetiology, our consultants at Evelina London Children’s Hospital (including our consultant in paediatric and fetal cardiology, Dr Owen Miller), recently led the world’s largest cohort study on PIMS-TS across 55 centres in 17 European countries to better understand the condition. Among other findings, it demonstrated that patients from a BAME background were most susceptible, with almost a third of patients with PIMS-TS in the study being from a black background.
In addition, obesity was a common comorbidity associated with the development of the syndrome, with a quarter of patients meeting this criterion. However, no other potential risk factors (including diabetes) were found to be associated. Interestingly, the study also revealed that a shorter period of symptoms before admission to hospital significantly increased the likelihood of a worse outcome and the requirement for extracorporeal membrane oxygen and/or death.
What should doctors look out for?
“What the study demonstrated is that it is essential to admit patients to an acute care centre as soon as possible with this condition, to ensure the best outcomes. It is hard to predict which patients will deteriorate most rapidly, but in the right setting they may be stabilised promptly to enable their recovery. Rapid accurate diagnosis is therefore key,” explains Dr Carles Bautista, our consultant paediatric and interventional cardiologist at Royal Brompton Hospital.
Clinical features of PIMS-TS
- aged 18 or under
- recent history (previous 4 to 6 weeks of COVID-19 infection or contact with infected individual)
- abdominal symptoms: diarrhoea, pain and vomiting
- conjunctivitis and/or widespread rash
- cracked lips and/or strawberry red tongue
- headache
- hypotension and/or dizziness
- lethargy and myalgia
- peeling on hands and feet
- prolonged high fever
- tachycardia +/- shock
Multi-disciplinary care is needed
As PIMS-TS can be a multi-system condition, a multi-disciplinary approach is needed for its successful treatment. Our consultants at Royal Brompton Hospital and Evelina London Children’s Hospital work in partnership to provide the best care.
With our expertise in heart and lung care, we can work quickly to diagnose the condition and stabilise the acute cardiac and respiratory problems associated with it. As the gastrointestinal system is also often involved as well as other systems, we tap into the expertise of specialists from across our hospitals for a total body approach to care.
Protecting Joseph’s heart
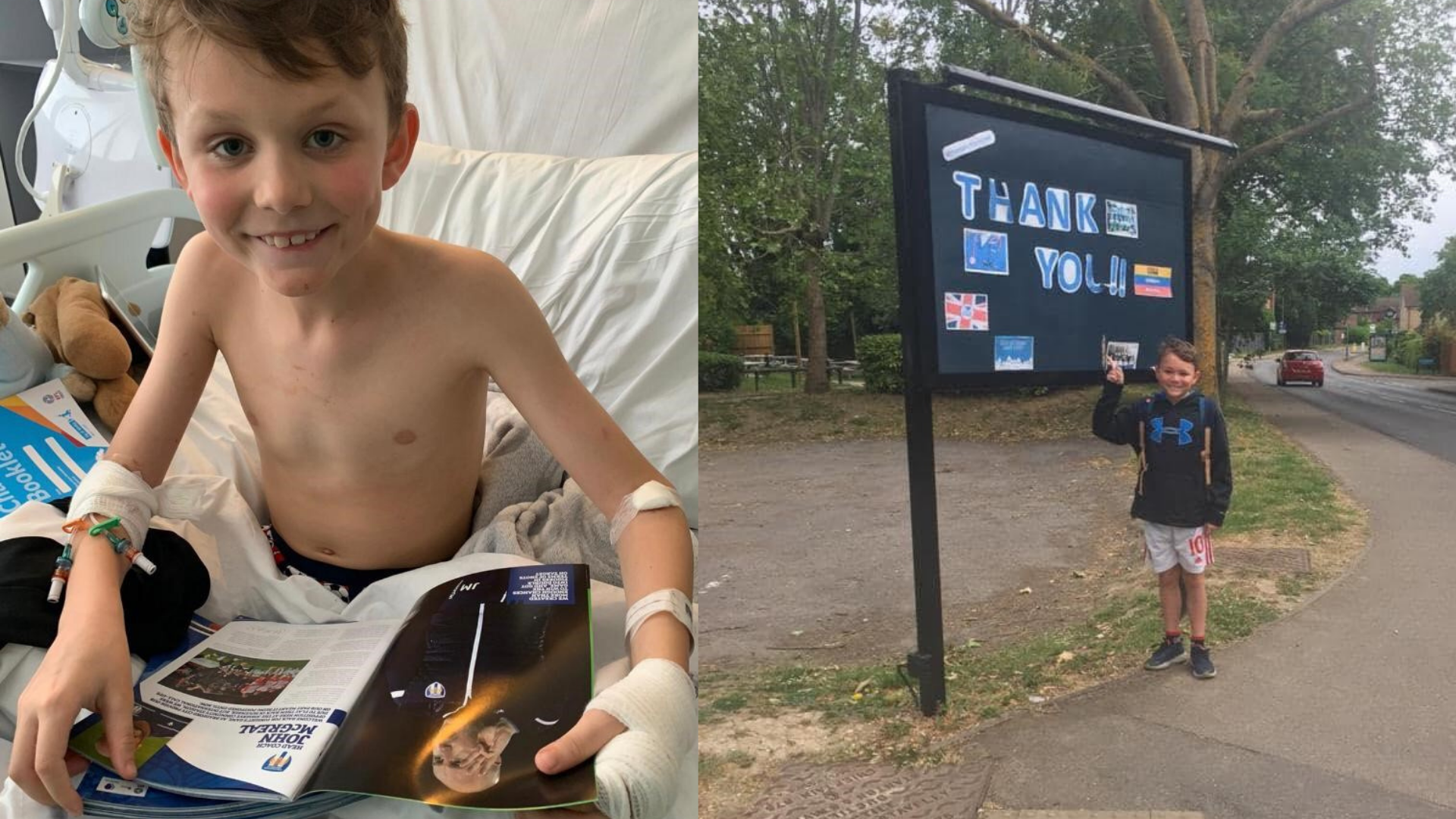
(L) Joseph recovering from PIMS-TS at St Mary's Hospital. (R) Joseph fully recovered and raising money for the NHS.
Joseph, aged 10, was experiencing bad tummy and back pain in April 2020. “He was a very healthy and sporty boy, playing football regularly and was rarely unwell, so I just immediately thought I needed to take him to A&E as this was really unusual for him,” explains Joseph’s mum, Elle.
“He couldn’t walk at all from the pain, so the doctors conducted some scans to see if it might be his appendix. He was also really sensitive to the hospital light and started developing a high fever which paracetamol wasn’t managing to bring down.”
The team at Princess Alexandra Hospital decided to keep Joseph in for further investigation, but his condition deteriorated rapidly. He received a positive test for COVID-19 infection and started showing signs of PIMS-TS, including a swollen strawberry red tongue and inflammation in his heart, prompting his transfer to St Mary’s Hospital’s intensive care unit for treatment.
“He was incredibly poorly and I just didn’t think COVID would affect his heart this way. But Dr Bautista was brilliant. He came to visit Joseph twice a day to check on and treat his heart. There are no words to describe how grateful I am to him and all the doctors and nurses at St.Mary’s and Royal Brompton Hospital in helping with Joseph’s recovery,” says Elle.
“It took Joseph a year to recover from his experiences in intensive care but he is now back to playing football again. He even raised over £1,000 for the NHS in a charity bike ride as a thank you for his treatment. We are incredibly proud of him.”
As PIMS-TS can affect multiple organs, a multi-disciplinary approach is needed for its successful treatment. Our paediatric cardiologists at Royal Brompton and Evelina London Children’s hospitals work in close partnership to provide the best care for patients. Together, they can provide a comprehensive service to quickly stabilise these very ill paediatric patients and utilise diverse specialist expertise for a total body approach to care.

