Around 15 million people in England live with chronic pain, with more than 5 million of those experiencing high-impact chronic pain that leaves them struggling to take part in daily activities. While pain levels vary, the most severe cases of chronic pain see patients bedbound and unable to work. Consultants at St Thomas’ Hospital are proud to offer a life-changing procedure, spinal cord stimulation, to treat chronic pain in these patients.
What causes chronic pain?
Our specialists at St Thomas’ Hospital offer spinal cord stimulation to patients with a variety of chronic pain including back pain, facial pain, cluster headaches and migraines, bladder and pelvic pain, neck and upper limb pain, interstitial cystitis, and pain following hernia repair operations. The cause of chronic pain varies depending on where in the body it occurs, but it can begin after surgeries, accidents and injuries, or simply occur due to a genetic predisposition such as is the case with migraines.
Chronic back pain is one of the most common types of pain, with an estimated 10 million people in the UK suffering from it, accounting for 11% of disability in the population. In the UK, 2.6 million people visit the GP each year for lower back pain. Chronic back pain commonly occurs after injuries from accidents such as falls or heavy lifting, which affect the back muscles, spinal ligaments and spinal discs.
As a society, we have increasingly sedentary lifestyles, resulting in more chronic back pain due to weakened, unused muscles, increased stiffness, and decreased flexibility. The recent shift to working from home is thought to have exacerbated this phenomenon, with disabilities caused by back or neck problems increasing by 62,000 more people between 2019 and 2022.
Of all types of chronic pain, lower back pain contributes to 24% of cases. The most common group of patients our specialists at St Thomas’ Hospital see are those with failed back surgery syndrome (FBSS). This is the term for spinal pain with no known origin, which previous back surgery was unsuccessful in treating.
Current pain management options
The standard treatment options for both FBSS and other types of chronic pain range from non-steroidal anti-inflammatory drugs and epidural steroid injections to physical therapy and opiate pain relievers. Sometimes, a combination of treatment options is required to make a difference in the patient’s pain level. In other cases, for reasons often unknown, the treatments have no effect or cannot provide a high enough level of pain relief. For these patients, spinal cord stimulation can block the pain signals.
Dr Adnan Al-Kaisy, consultant in pain medicine at St Thomas’ Hospital, led the first multicentre and multinational study on the safety and efficacy of spinal cord stimulation in managing FBSS. He also regularly treats patients with other types of chronic pain. Spinal cord stimulation works by targeting the nerves on the spine, which transmit pain signals to the specific area affected by the pain.
What is spinal cord stimulation?
The Pain Management and Neuromodulation Centre at St Thomas’ Hospital is home to the largest pain centre in the world. With about 100 department employees, our hospital is one of just 5 centres nationwide that offers spinal cord stimulation, regularly pioneering new techniques in the neuromodulation speciality.
“The term ‘spinal cord stimulation’ is nothing new,” explains Dr Al-Kaisy, “as it’s been around since 1967. However, the technique has evolved over the last few years thanks to advancing technology, which has given us a better understanding of the pathophysiology of different pain conditions.”
Spinal cord stimulation, first pioneered at St Thomas’ Hospital, is an alternative to major surgery and the other aforementioned standard pain management options for chronic pain, from NSAIDs and epidural steroid injections to physical therapy and opiate pain relievers. Our team of specialists now perform spinal cord stimulation an average of 200 times a year.
The treatment works by delivering small electrical currents to the spinal cord through implanted electrodes, disrupting pain signals and preventing them from reaching the brain. It consists of inserting a small, specialised wire into the epidural space very close to the nerve, and the treatment is delivered by a lead connected to a matchbox-sized battery-powered generator.
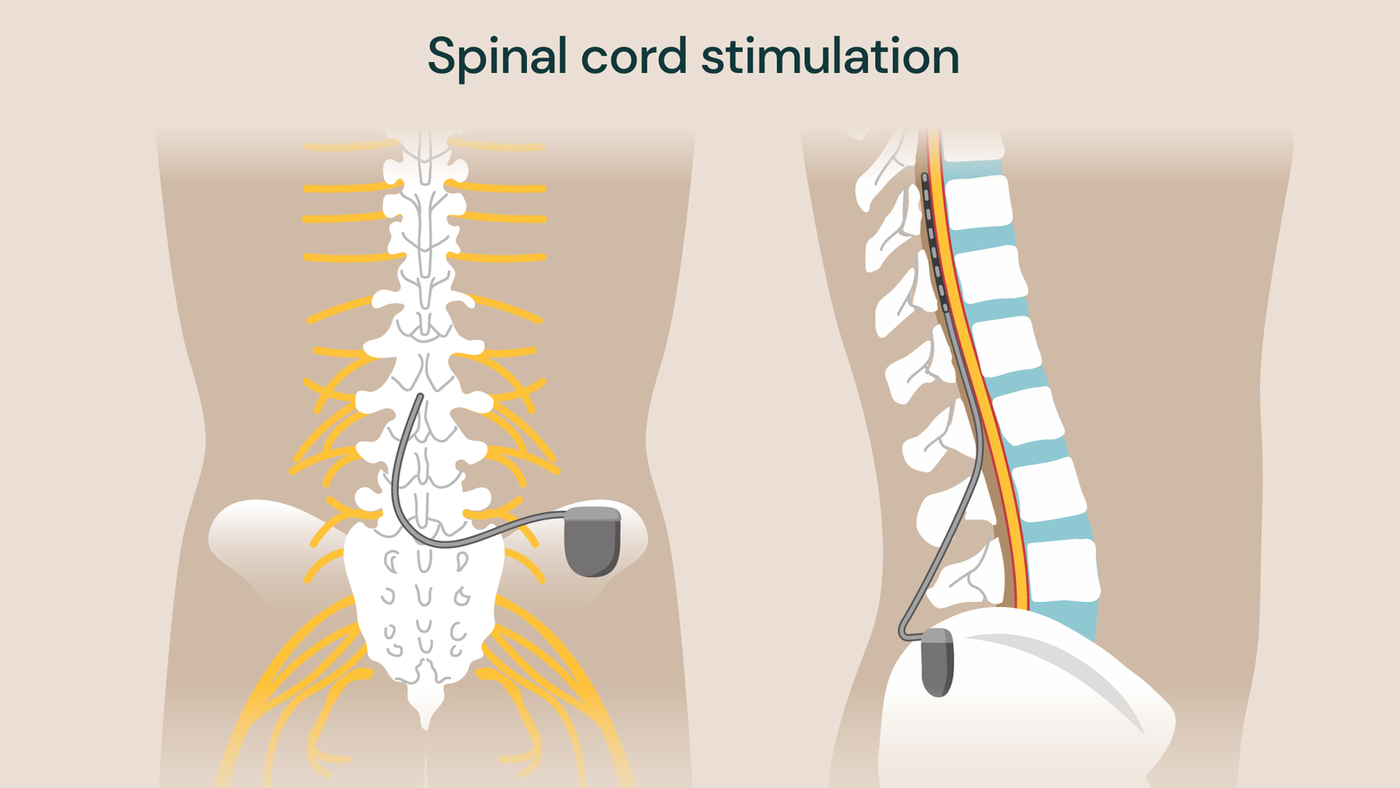
Spinal cord stimulation shown with the implanted electrodes attached to the spine, and the generator device at the base of the spine
“The patient will be provided with a remote to control the stimulation of the spinal cord to reduce their pain,” explains Dr Al-Kaisy. “They can turn spinal cord stimulation on and off so, in essence, the patient will control the pain rather than the pain controlling the patient.”
The battery that powers the generator is rechargeable, lasting for around 5 years, and can be charged every few days by putting an antenna on the battery to charge it through the skin. Other non-rechargeable batteries can last 4-5 years before requiring replacement with a small procedure.
Benefits of spinal cord stimulation
Dr Al-Kaisy summarises the procedure’s benefits as “minimally invasive, simple, and reversible.” To assess its effectiveness, he and the team at St Thomas’ followed 21 lower back pain patients (who had never undergone spine surgery before) for 3 years after having the device implanted. The findings were clear: the overall intensity of the patients’ pain had reduced by 80%, 75% of patients were able to return to work, and 90% had stopped taking opioid medication.
“The patient satisfaction and social aspect is high, and the complications were very small,” explains Dr Al-Kaisy. Patients’ families, friends and employers also benefit from the patient being pain free as, in most cases, they can resume many of the daily activities and work that chronic pain forced them to give up. Most patients can also stop taking pain medications which may have caused negative side effects.
Spinal cord trauma after device implantation is a very rare complication, occurring in 1 in 300,000 cases.
When to refer to us
Patients with chronic pain can be referred to us for spinal cord stimulation. Patients who may be unsuitable for treatment include those with localised knee, hip or joint pain, as these are examples of mechanical pain resulting from the joint itself, and therefore will not benefit from the implant. Patients can be referred from the age of 18 with no upper age limit.
Get in touch
For more information on spinal cord stimulation and pain management services at St Thomas’ Hospital, please contact our customer services team.
